
Wellings and Alpers 17 examined the frequency and age distribution of apocrine cysts in normal women versus women who developed cancer in the same or contralateral breast. 15 This prompted Eusebi et al 16 to conclude that apocrine features should be considered a normal change in breast epithelium rather than a true disease. 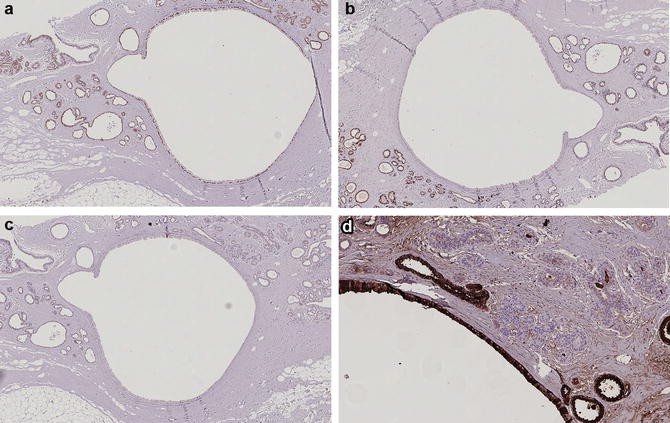
The incidence of apocrine cysts found in normal breasts obtained from autopsies is said to be as high as 85%. 12, 13 The study by Tsung et al 14 revealed that apocrine cells were present in both type I and type II cysts and that cyst type could not predict the likelihood of subsequent carcinoma development. The current consensus is that gross cysts are not associated with any significant increased risk of subsequent carcinoma development, therefore these women do not require any further follow‐up than would be offered routinely. 
10, 11 However, two of the largest studies with long term follow‐up showed conflicting results. 9 Women with palpable cysts who have undergone aspiration, have been reported to have a slightly increased risk of subsequent carcinoma development. There was initial evidence to suggest that type I cysts had a higher likelihood of recurrence than type II cysts, 7, 8 but this has not been reproduced in studies with larger numbers of patients and longer follow‐up. The cyst lining was found to be closely related to the content, where type I cysts are usually lined by apocrine cells and type II cysts are usually lined by flattened epithelium. Lower concentrations of sex hormones and epidermal growth factor are also a feature of type II cysts. Type II cysts have high concentrations of sodium and chloride and low concentrations of potassium (K:Na ratio <1.5). High concentrations of androgen and oestrogen conjugates and epidermal growth factor are also present in this type. Type I cysts have a high concentration of potassium and low concentrations of sodium and chloride (K:Na ratio >1.5). Miller et al, 5 categorised cysts into two types based on their electrolyte content. These cysts can be microscopic or grossly visible. 6 Formation of cysts is one of the basic morphological criteria of this disease. In addition to carcinomas with obvious apocrine differentiation, other carcinomas have some apocrine features and it may be that a significant number of breast tumours arise from apocrine epithelium or that a significant number can express some apocrine features.Īpocrine metaplasia in fibrocystic changeįibrocystic change is an extremely common finding, which is evident in about 50% of women of reproductive age. Fibrocystic change, fibroadenomas, hamartomas, papillomas, sclerosing adenosis and apocrine adenoma are all benign breast lesions that can show apocrine change as one of their histological features.Īpocrine lesions can be divided into simple and papillary apocrine changes, those of uncertain significance, those found in association with other lesions, apocrine ductal carcinoma in‐situ and invasive apocrine carcinoma. Not only are some of these lesions difficult to categorise, but also there is controversy regarding their relative risk of subsequent carcinoma development. 5Īpocrine change in the breast is seen in a broad spectrum of lesions ranging from microscopic cysts to invasive apocrine carcinoma. The mechanism for the development of apocrine metaplasia from normal cuboidal epithelium is not well characterised, but it is a pathognomic component of fibrocystic change and in type I breast cysts. One of the reasons, however, that these are often not regarded as normal components is that examples of gradual metaplastic change from the normal cuboidal epithelium can be seen and cells with intermediate features can also be discerned on careful examination, suggesting that these are true metaplasia (fig 2 2). Metaplastic apocrine cells within the breast are similar to normal axillary, areolar and perineal apocrine cells, having apocrine secretions and identical staining reactions. 4 GCDFP15 is identical to prolactin inducible protein, GCDFP24 is apolipoprotein D and GCDFP44 is zinc α2 glycoprotein. 2, 3 They also stain with three proteins found in cyst fluid, called gross cystic disease fluid protein (GCDFP) 15, 24 and 44. Normal apocrine cells do not express oestrogen (ER) or progesterone receptors (PR) but are positive for androgen receptors (AR). H&E.Īpocrine cells stain with periodic acid‐Schiff after diastase digestion and are immunoreactive for epithelial membrane antigen (EMA) and cytokeratins 8 and 18. Figure 1 Apocrine metaplasia within fibrocystic change.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
